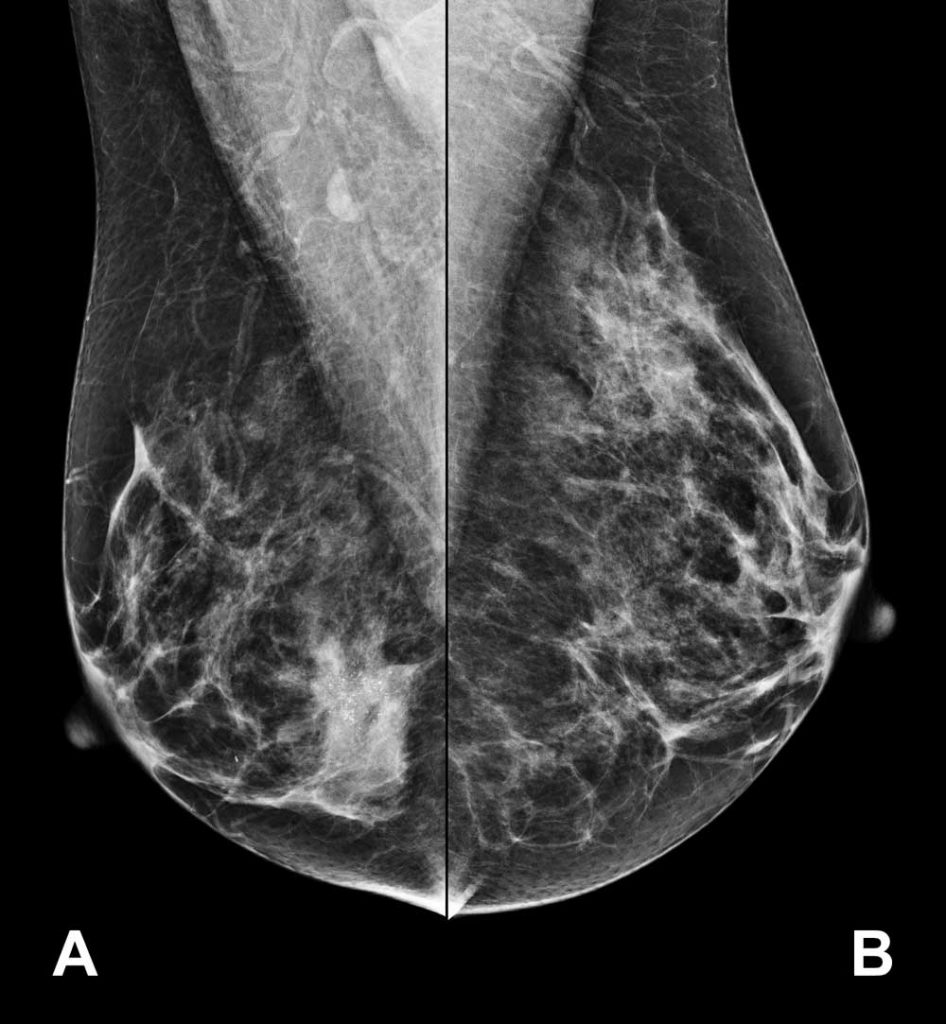
Breast cancer screening
As previously mentioned, the establishment of population-based screening programs has helped to reduce mortality from breast cancer, due to the fact that they enable diagnosis of the disease in its earlier stages. The current recommendations from the U.S. Preventive Services Task Force on breast cancer screening are:
1
To perform a mammogram every two years on women between the ages of 50 and 74.
2
The benefits of applying the screening program to women over the age of 75 are not well established.
3
Mammograms for breast cancer screening should not be given to women between the ages of 40 and 49. Their implementation in this age group should be assessed on a case-by-case basis.
4
There is insufficient current evidence to recommend scans additional to mammograms in women under the age of 40.
The recommendations for women between the ages of 40 and 49, as well as the frequency with which mammograms should be performed, have created significant controversy. Therefore there may be modifications to these general recommendations in different geographical areas, the most common alternative being the performance of an annual mammogram from the age of 40.
Several studies seem to support alternating mammograms and breast MRIs every six months in women who have an identified BRCA1 or BRCA2 mutation, as this reduces the number of breast cancer cases diagnosed in advanced stages. However, the use of breast MRI outside this group of patients is not recommended.